Healthcare: No End In Sight – Poor Value at Unsustainable Costs
Something is seriously wrong…
The healthcare industry as a whole in the United States is corrupt, dysfunctional, ineffective, and inefficient. And regardless of “party affiliation”, everyone appears to share this opinion. The only real disagreement (and a heated disagreement at that) is what should be done about it, and whether what has been done to date has a chance of working as promised over time.
This article is pragmatic, not political. It contains anecdotes of my experiences as a recipient of healthcare in the United States versus Germany. It also contains my experiences and findings in the pursuit of adequate health insurance and the costs of healthcare delivery. And lastly, it will contain some reasonable (at least I believe they are reasonable) first steps for improvement.
I am going to start by sharing some of my personal anecdotes about the experiences I have had with the healthcare industry over the years.
Jonathan’s Foot:
My first son, Jonathan, was born with slightly deformed feet. We were referred to an Orthopedic Doctor for consultation and treatment. The doctor’s diagnosis was that Jonathan had a marginal case of “clubbed feet” as per an analysis of some x-rays and the prescribed treatment was either a serious of casts (similar in effect to having braces on the teeth), or surgery, to correct the problem. Naturally, we selected the less invasive approach, but over the coming months, the doctor started to press for the surgery. Having our doubts, we decided to obtain a second opinion from a doctor in Sayre (Pennsylvania) who was not affiliated with the medical “ecosystem” where we lived in Binghamton (New York), as we did not want a chance of “bias” in the opinion.
The second doctor confirmed the first doctor’s diagnosis, but kept hedging when we asked for a recommended course of action. I could tell he was not very keen on surgery, but I could not get him to say anything definitive.
Finally, I asked the magic question, “Hypothetically, Doctor; if this were your son, would you or would you not have the operation.” Almost relieved, the doctor looked at me and responded, “Hypothetically, if it were my son, I would not have the operation.”
“Thank You, Doctor!”
Finally, I get an honest (if indirect) answer. But, why couldn’t he just say that?
Result: Jonathan did not have the surgery. We continued with the casts from the first doctor until the first doctor became unbearable, and then we stopped. Jonathan grew out of the condition by the time he learned to walk (reasonably on-schedule) and now is without any problem.
Cape May Experience:
Once whilst on a family vacation in Cape May (New Jersey), Jonathan got sick on some shrimp that he had for dinner. We were sitting in the hotel room debating the course of action as Jonathan vomited in a waste-can. With short order, it was decided to take him to the hospital in case it was an allergic reaction.
It was about midnight by the time we left the hotel and traveled to the hospital. Except for the receiving nurse and us (and the waste-can), there were no other people when we arrived at the Emergency Room. We were asked to wait and told that “someone will be with you momentarily”.
We waited for about fifteen (15) minutes – during which time, nobody else came or left from the reception area. The reception nurse looks up from her computer screen and asks us to come over so she can enter our arrival into the system. She takes our basic information and the nature of the situation and enters it into the system. Afterwards, she asks us to wait and says that “someone will be with you momentarily”.
So we sit back down for another thirty (30) minutes – it’s now almost 1am and nobody has come or left from the reception area. Again, the reception nurse looks up from her computer screen, pivots 90-degrees, slides-open a glass window, and asks us to come over so she can enter some additional information into the system. Afterwards, she asks us to go through a door that is right behind us, sit down, and wait; “someone will be with you momentarily”.
We sit there for another thirty (30) minutes. Finally, someone comes to us with a clip-board, guides us to a bed, pulls the curtain, and tells Jonathan to take his clothes off and slip into a robe and, “someone will be with you momentarily.” – Yeah, I get that. And since he never introduced himself, I never knew if the person was a doctor or a nurse (heck, he could have been the janitor for all we knew).
After the “dude with the clip-board” leaves, I look at Jonathan and tell him, “Never mind what he said. Don’t get undressed. Who knows how long we will be here.” So the two of us, and the waste-can, sit on the bed for almost another hour without anyone coming to see us. And all during this time, I did not see any other patient or hospital staff – only one police officer (I don’t know why he was there – we never spoke).
It’s now almost 230a. I look at Jonathan and he looks at me. I ask him, “Are you feeling better? Do you feel like you’re going to die?” He responds that he feels fine, but tired.
“Let’s get out of here… Leave the waste-can.” And we leave.
Later, I get a “bill for emergency services rendered” from the hospital. I write them a letter telling them my story and how there are no circumstances where I will ever write them a check or even submit the bill to insurance – they did nothing and they deserve nothing. They respond by “forgiving” the bill.
My Umbilical Hernia:
One day this year (May 2012), I am sitting at my desk in Seligenstadt Germany when I notice a small protrusion from by naval. When I push it, it goes back inside my abdomen. It doesn’t hurt, but it does take me by surprise and make me feel very squeamish and ill-at-ease. With a little internet research, I self-diagnose an “umbilical hernia” and start looking into the possible causes, remedial action, healing process and long-term prognosis. Having this information, I then call a friend in the United States who is a doctor and discuss my findings. She concurs with my diagnosis and reinforces what I found in my investigations that; “This won’t heal itself. It will only get worse over time. And you should look into having it fixed the only way it can be fixed – surgery.”
So back to the internet I go. I have two options; 1) find a surgeon and a hospital here in Germany which can fix me, or 2) find a surgeon and a hospital back in the United States which can fix me. After careful consideration, I decide to give Germany a chance and start looking for a surgeon and hospital who can sort me out – speaking English is a requirement. A search on the internet identifies several potential candidates, with one being in nearby Wiesbaden, which is about 45min away and home to one of the few remaining US Military bases still in Germany.
I make an appointment with the doctor at the hospital for a consultation in early June. Everything is well-orchestrated and precisely on-time. I arrive about 30min early and the receptionist logs me in and has me fill-out a couple forms which contain just the most basic of information;
- Name, Address, Telephone Number, Nationality.
- Insurance or Self-Pay (I am considered self-pay since my health insurance is in the United States. I have to pay for the services; then submit my bills to my insurance company for reimbursement).
- Nature of the ailment
- Anything about my health or diet that might be important for the doctor to know.
I meet with the doctor as scheduled. It’s a fairly brief appointment because I already know the problem and its nature; I have some ideas as to how it will be fixed and the various options that are available, and what to expect for healing. After all of this has been discussed, we decide to schedule the surgery for mid-July after his vacation. Remember, it’s not a situation that requires immediate attention, it just needs attending. Besides, I have sailing the Aegean in late June and I can’t miss that!
The day comes for my surgery. I arrive in Wiesbaden the day before my surgery for the pre-operative tests and physical and to “meet the surgical team”. The surgeon says that the hernia is only less than 5mm in size and that he will probably not need to insert a mesh. I ask if getting a “local anesthesia” instead of a “general anesthesia” is a possibility. He seems surprised (crazy Americans), but then I explain that; I don’t like the idea of being put to sleep, I don’t like how I feel when I wake up (I feel like crap for a day or more), and it just adds to the possible complications. He and the anesthesiologist confer and agree to give me just a local anesthesia.
The day of the surgery, I arrive at the hospital at 7a as scheduled. I go to pre-op, get ready and wait for my turn. I end-up waiting for a long time. Evidently, there were a few emergencies that “bumped me” in the schedule, but the staff was very good at keeping me informed. At around 11a, they asked if I wanted to be fed intravenously (IV), as I had not eaten since the previous evening. My turn finally comes around 3p and I am wheeled to surgery.
Once I get to the operating room, I notice that it is staffed with the surgeon, the anesthesiologist and three nurses. It is very clean and orderly (as I would expect), but I can’t tell how modern it is (after-all, it’s not my profession). The doctor and I engage in some minor chit-chat and he introduces me to the others in the room and their roles and we prepare for surgery. I ask about an IV (I never heard of a surgery without an IV) but he tells me there is no need. I also ask about an antibiotic in case of infection – the doctor tells me an antibiotic is not necessary. Okay, what do I know?
Even though it is a local anesthesia, I can still feel the tugs and there is some twinging. I try to concentrate on something else and start rubbing my thumbs in my hand to help take my mind off of what I am feeling. Then, one of the nurses – a very attractive nurse with blue eyes and longish blonde hair – sees this activity and asks how I am doing. She sits down next to me, holds my hand, strokes my forehead, and starts talking with me. Way-cool, my mind is no longer on the surgery.
After 45min, I am out of surgery and being wheeled to my semi-private room. The room is set up pretty nice. The television is rather small and far away, but it doesn’t really matter since the programming is all in German. I ask if the hospital has WiFi that patients can access – and sure enough, it does. I am on-line! Between the internet and my Economist magazines, I can last for days!
Later on, the duty nurse comes-by to check on me and asks what I would like to eat (remember, I had not eaten since the evening before). I let him know that I could really go for a pizza and a wine; he laughs and tells me he will check with the doctor – I am thinking, “Yeah, right. Sure you will.”
But a little while later, he comes back and says the doctor has approved the pizza and wine! So, that night I have a plain pizza and split of red-wine (375ml) for dinner. Wow, I am in the hospital; connected to the internet, doing my work, catching-up on eMails, having Skype-calls, reading the news, having pizza and wine – all the while being attended. If the sponge-bath comes with a “happy ending”, I am never leaving. I never did find that out.
Although this would be an “out-patient” procedure in the United States (in and out the same day, if there are no complications), I am scheduled to spend two nights in the hospital. I am worried about the cost.
Then it dawns on me; they never secured any method of payment prior to rendering services. I have no insurance recognized in Germany and marked as self-pay; which means that I am personally and solely responsible for the payment for services rendered and they have no recourse to others. They did not ask for a deposit, or a credit-card, or an auto-payment from a bank account. Heck, they didn’t even ask for identification! I could have said I was Jurgen Zaiser at Willy-Brandt-Straße 1
10557 Berlin (Angela Merkel’s address) and they would have never had the opportunity to know otherwise. Try having THAT experience at a hospital in the United States.
Almost six weeks later (the end of August) I receive a single bill for the services rendered. A summarized bill of services rendered:
- Pre-operation consultations and tests.
- Operation with a surgeon, anesthesiologist, and three nurses for one-hour.
- Post-operative care and monitoring.
- Two nights in a semi-private room with WiFi.
- TOTAL: e2,900 (or $3,750). Are you kidding me!? Including holding my hand?!
I was very surprised at how little all of this cost and called my doctor-friend in the United States about it. After describing what I received, she told me the cost for the same in the United States would be between $20,000 and $25,000.
Are you kidding me? How can that be?
So It Gets Me Wondering:
1) It appears the cost of delivering healthcare in the United States is far greater than the cost of delivering healthcare elsewhere – is this true?
It has already been anecdotally established that the costs for the healthcare services I received in Germany is approximately 60% less than what I can expect in the United States. But how can this premise be extrapolated so that it supports a more general statement regarding the cost of healthcare?
It’s that time of year again when I start evaluating the group health insurance plans for value (defined as cost of the premium versus coverage received – with a fudge-factor in there for the amount of the deductible). It appears that the monthly premiums in 2013 will be $500 (single) and $1,200 (family) – with a $1,500 deductible ($4,500 family maximum). One of my frustrations is that I presently have to purchase health insurance from New York (since it’s the only mailing address in the United States that I have). The very same policy, from the very same company in Illinois, would cost me a minimum of 25% less. So, instead of paying $1,200/month for a family policy (as I do), I would be paying $900/month or less (a minimum of $300/month savings). Since my health insurance policy allows me to obtain the healthcare services in any State (or even country), why can’t I purchase my health insurance from any State?
One of the intents of the Patient Protection and Affordable Care Act in the United States (also referred to as “Obamacare”) is to reduce the cost of healthcare delivery so that it is affordable for everyone. A major part of the plan to accomplish this is to mandate that everyone in the United States purchase Health Insurance – and one would think that fostering a competitive market for health insurance would result in lower premium costs and higher benefits as insurance companies vie for customers and market share. However, Obamacare does not allow for competition across State-lines, with the result being a stifling of healthcare insurance options.
Representative Paul Broun, MD (Republican, Georgia) introduced a Bill (HR 4224) entitled “Offering Patients True Individualized Options” (OPTION). This bill was introduced as a “repeal and replace” bill to Obamacare, which means that it had no chance of ever passing. However, there were some ideas in there worth considering of incorporating into Obamacare to reduce the cost of obtaining and retaining healthcare insurance, containing the costs, and improving the coverage – including the ability for people to purchase their health insurance from any company in any State AND the ability for smaller businesses to band together and thus be able to negotiate a lower cost.
So given these frustrations with the cost of health insurance, and the overwhelmingly positive experience I had with my healthcare services delivered in Germany, I decided to look for an “Expatriate Health Insurance Policy” designed for people like me. Of course, the policy had to be from a reputable company (it serves no useful purpose paying very little in insurance premiums if the company will never pay on a claim).
One of the first hits on “Google” was “Allianz”. I reviewed their plans and found them to be very comprehensive in their coverage as compared to those I have had in the United States – especially if the “Core-Plan” were supplemented with the “Out-Patient Plan” – in fact, I believe the coverage is superior to the plan I currently have.
After typing in my basic information (family members, ages, etc…), selecting the “Classic Individual Core Plan” and selecting a e750 deductible (approximately $1,000 as compared to the United States-based plan of $1,500) for which I receive a 10% discount from the list rate, I was given the this offer:
- e4,845 Annual Premium (which is $6,250 Annual or $525 per Month).
- Treatment from any medical provider of my choosing anywhere in the world.
A bunch of “companion” benefits that don’t exist in a typical United States-based insurance policy.
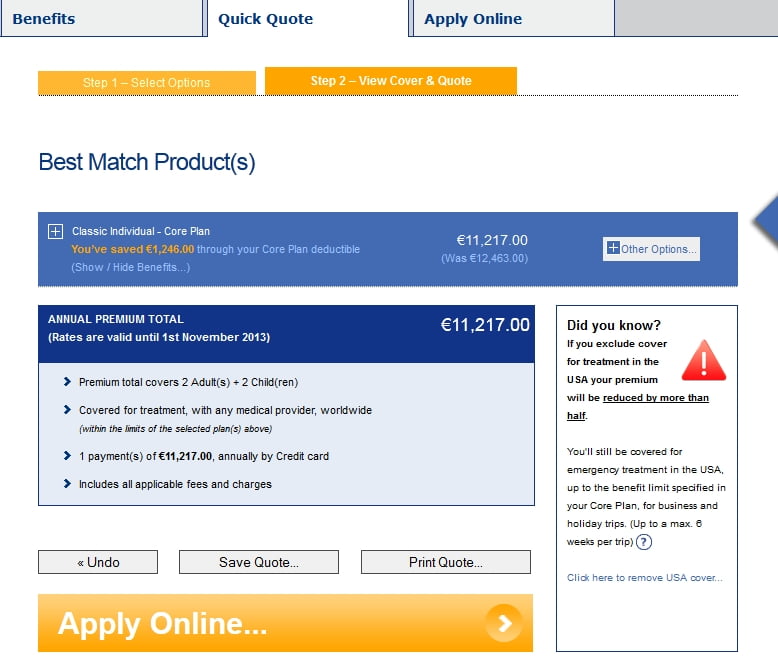
But I noticed something strange, that there was an exclusion of the United States from where I could get services rendered. So, I looked at how I might get the opportunity to include the United States and this is what I received as an offer, e11,207 per year – a full 225% more than the offer which excludes the United States (or 325% of the original offer).
But, Allianz was kind enough to warn you of this (see big red triangle with “!”) and telling you that the saving can be “reduced by more than half.”
Allianz went on to say that you would “still be covered for emergency treatment in the USA, up to the benefit amounts in the Core Plan, for business and holiday trips – up to a maximum of six (6) weeks per trip.” The only thing that can be safely inferred as a result of my anecdotal experience and this insurance offering from Allianz is that healthcare delivery in the United States costs more than twice as much as in other developed countries. So it looks like Allianz’s stance is that they will cover your healthcare services in the United States if you are already in the United States and have an emergency, but you can’t select to have healthcare services rendered in the United States if you are outside the United States without incurring a huge increase in insurance premium.
NationMaster, which bills itself as;
“a massive central data source and a handy way to graphically compare nations. NationMaster is a vast compilation of data from such sources as the CIA World Factbook, United Nations (UN), and Organization for Economic Cooperation and Development (OECD).”
… shows that the United States (at 15.4%) spends more on healthcare, as a percentage of Gross Domestic Product (GDP), than of any other country of 188 countries reported. Most of the European and G20 countries spend between 9.0% and 10.5% of GDP on healthcare (with Japan ranking #45 at 7.8%).
And the United States also spends the most per-capita (at $6,100). Most European and G20 countries spend a full one-third to one-half less per-capita than the United States.
So this is not just a personal perception based on personal anecdote and an insurance quote, this is a fact – the United States spends a magnitude more on healthcare than any other country in the world.
2) If the cost of delivering healthcare in the United States is far greater than any other country in the world, are the results that much better?
We established that healthcare in the United States is the most costly in the world. But does that matter as much if the quality of the delivery, and most important, the outcome for services rendered, is also better than can be found anywhere else?
One way of determining the quality of the healthcare delivery would be to investigate the number of negative consequences that might be indicative of poor healthcare delivery. One way of measuring negative consequences would be to evaluate the number of infections that occurred during the delivery of healthcare.
One such infection, which is closely tracked world-wide is Methicillin-resistant Staphylococcus aureus (or MRSA) – a bacterium responsible for several difficult-to-treat infections in humans. I was unable to find an analysis of MRSA which originated solely in the delivery of healthcare, but this chart from the CDDEP shows that the United States has some of the highest incidents of MRSA in the world, worse than “Latin America” as a whole.
How can a person rationalize that the most expensive healthcare system in the world also has the highest incidents of infection from a bacterium?
If we take a look the OECD’s “Better Life Index” (which is a fascinating multi-dimensional analysis, by the way of looking at overall quality of life), we can compare “Health” in the United States with that of thirty-five (35) other countries (including those in the G20).
Of the 36 countries ranked for “Life Expectancy”; the United States was ranked #27 at 78.7 years average life expectancy (keep in mind that Social Security kicks-in at 65 years – food for thought for another discussion). The breakdown for this average was a life expectancy of 81 years for women and 76 years for men. Both the total average age, and the average age for both women and men, is below the OECD average.
Some other findings in the OECD analysis:
– The United States spends two and one-half times (2.5x) as much on healthcare as the OECD average including such countries as Germany, France, the United Kingdom, Canada and Japan.
– The United States is the “fattest country” in the OECD, with 33.8% of adults (and 40% of children) considered obese as compared to an OECD average of 14.9%. This results in extraordinarily high rates of chronic disease such as diabetes, cardio-vascular diseases and asthma. Reuters reports that the Center for Disease Control (CDC) projects an obesity rate of 44% in every State by 2030.
 Interestingly, people in the United States “self-reported health” at 90% “good” or “very good” which was the highest in the OECD analysis, where the average was 70%. This is in response to the question posed to individuals, “How is your health, in general?” How can a people who suffer more chronic disease and with a lower life expectancy claim they are healthier than their statistically healthier peers? Do they actually feel better? Perhaps they expect less? Or maybe they are more optimistic?
Interestingly, people in the United States “self-reported health” at 90% “good” or “very good” which was the highest in the OECD analysis, where the average was 70%. This is in response to the question posed to individuals, “How is your health, in general?” How can a people who suffer more chronic disease and with a lower life expectancy claim they are healthier than their statistically healthier peers? Do they actually feel better? Perhaps they expect less? Or maybe they are more optimistic?
In addition to life-expectancy, another way of measuring the quality of healthcare would be in the measurement of “healthy years”. These are the number of years that a person can expect to a live full, active, and productive life without being unduly confined or restricted.
This chart from NationMaster compares the “life-expectancy” in “healthy years” of top developed countries, including those in the G20. I could only show the top “25” here in this graphic.
The chart illustrates that although the United States has the most expensive healthcare system in the world (by a considerable magnitude, however measured), in the quantity of healthy years that a person can expect, the United States ranks #22 (at 67.6 years) – behind almost all of the other G20 countries; and where you can expect an average of three years additional (or 5%) of “healthy years”.
I don’t see how it can be argued otherwise than specifying that the United States has, by far, the most costly healthcare system in the world – and the results are below-average. I would be very pleased to report a learned rebuttal.
3) And finally, what value is a patient receiving for the healthcare provided?
I am not just referring to the quality of the outcome, but the level of aggravation and frustration that must be endured up to, and including, the receiving of the healthcare. Is asking for and receiving healthcare as comfortable as it could be?
There used to be a day in the United States when healthcare had a very “personal” touch, where the “family physician” was a reliable and trustworthy advocate for the patient and where the doctor-patient relationship was unimpeachable. The doctor would not be afraid to speak his mind and freely offer a detailed opinion. There was an interest in the context of the patient; where the patient lived and worked, his family history (probably also known to the doctor), the current situation of the patient’s circumstances, etc… The doctor KNEW the patient.
But ever since the 1950’s, the bonds of this relationship have incrementally deteriorated to the point where the doctors are trusted no more than the insurance and pharmaceutical companies, the attorneys, and the government. In fact, they are almost all viewed as one and the same. The New York Times printed an article on July 29, 2008 by Tara Parker-Pope entitled, “Doctor and Patient, Now at Odds”, which gives an account of this decay in trust.
If doctors are more concerned about being sued (deservedly or not), remaining in the good graces of the insurance companies (both those for healthcare delivery and for malpractice), and/or having their compensation cut and limiting their income (thereby increasingly becoming corruptible to those with whom they might benefit financially) – then who is going to be the patient’s advocate and trusted advisor? Will the patient have a first-reaction of going to the doctor when something “isn’t right”? Or will the patient try to “wait it out”, see if it “goes away”, or try some “alternative medicine”. It didn’t work-out so well for Steve Jobs.
In my opinion, this is a primary focus-point if the quality of healthcare is to be increased and the cost of healthcare delivery is to decrease. The system has to be re-engineered so that patients trust their doctors, know they are going to get personalized services rendered (in context to the circumstances of the patient), know the treatment advice is trustworthy and unbiased, and know that the doctor is the patients advocate.
This is not the way it is today (regardless of any rebuttal) – but it needs to be.
Costs, Waste, and What is Being Done:
Going beyond the personal anecdote and what Allianz might think, an October 28, 2012 article in Reuters (a news service) entitled “Analysis: Employees to face healthcare sticker shock” and written by Caroline Humer, it is reported that employers in the United States are being forced to pass the spiraling cost of providing health insurance and healthcare services to their employees. This includes: contributing more towards their insurance coverage, higher out-of-pocket deductibles, eliminating coverages not required by law, and higher co-pays for routine appointments and prescriptions.
This trend across all companies in the United States (a trend for which I will be a participant), is demonstrative that the Patient Protection and Affordable Care Act is not satisfactorily accomplishing its intended mission – making healthcare affordable for all, and to have universal coverage. In my opinion, the Act is seriously deficient and will do more harm than good if the deficiencies are not immediately addressed.
But please don’t confuse the above statement with my wanting to eliminate the Act; or otherwise abandon it (or its intent). I believe a “National Healthcare Policy and Program”, properly engineered and deployed, is the first step towards reducing costs (largely by reducing waste) and simultaneously increasing the quality of the results. I believe this can be accomplished as a re-engineer from within the existing framework of Obamacare.
However, obtaining universal health insurance coverage is only part of the solution. The costs associated with healthcare delivery continue to spiral out-of-control and must be contained (even rolled-back).
 The Economist published this graphic demonstrating the amount of ANNUAL waste that exists in the delivery of healthcare in the United States – an estimated total of between $600 and $850 BILLION DOLLARS ANNUALLY.
The Economist published this graphic demonstrating the amount of ANNUAL waste that exists in the delivery of healthcare in the United States – an estimated total of between $600 and $850 BILLION DOLLARS ANNUALLY.
Of this annual amount, approximately 37% is classified as “unnecessary care” – meaning delivered, but not needed.
The source of the data for the graphic was an analysis and subsequent article published on October 26, 2009 by Reuters entitled “Healthcare System Wastes up to $800 Billion a Year.” In it, it revealed that the primary sources of “unnecessary care” included the overuse of antibiotics (perhaps also leading to an increase in the instances of MRSA as noted above) and excess lab tests to protect against malpractice. A follow-up article by Reuters published on June 14, 2010, entitled “Key Cuts to Healthcare Waste Saves $3.6 TRILLION” identified several initiatives which would realize this reduction in costs over a ten (10) year period. These initiatives included: an increase in personal awareness to risk the responsibility for one’s lifestyle, creating “bullet-proof” checklists for processes and procedures to reduce mistakes in healthcare delivery (similar to a “pre-flight checklist” used by pilots), increasing patient awareness in their responsibility for eliminating fraud and to take an active role in the delivery of their healthcare, and changing the “reward system” for healthcare providers from “inputs” (i.e. delivery) to “outputs” (i.e. results).
For Your Consideration; First Steps for Improvement:
1) National Base-Line Health Insurance Coverage
The very first thing that needs to happen is that there is a minimum standard for Health Insurance Coverage established nation-wide and every single person in the States (100%) is enrolled in the program (universal coverage) and there is no opportunity to not be in the program (no “opt-outs”).
There must be an emphasis on preventative care. And to encourage people to use it requires that the delivery of this care being made as simple, easy and pleasant as possible. As part of preventative care, patients should be educated on life-choices they make which will affect the state of their health – and there should be monetary incentives (perhaps reductions in premiums) for living more healthily.
And the Base-Line Insurance Coverage should cover (without co-pay);
- All non-work-related emergency services (work-related healthcare is covered by “Worker’s Compensation” insurance).
- All life-threatening situations including the treatment of chronic disease and conditions.
- It should not cover any non-life-threatening conditions or disease except to the extent that their early treatment would prevent them from becoming life-threatening.
But remember, “Somebody pays the party”. There is no such thing as “free”.
I would propose that this basic healthcare coverage should be paid by a tax collected specifically for his purpose. I personally believe an expansion of the FICA/Medicare tax is the most workable and spreads the cost of insurance evenly between employee and employer.
2) Opportunity for Premium Insurance Supplements
This national healthcare base-line coverage will not be designed to give everyone unrestricted access to any medical procedure, pharmaceutical or therapy. The national policy cannot be an “all you can eat” – all the healthcare you can want and whenever you want it. Therefore, there should be the opportunity for individuals to purchase supplemental (private) insurance which can provide enhanced services – additional therapies, perhaps non-generic drugs, discretionary procedures, access to specialists for non-life-threatening conditions, etc… Perhaps these policies can be a roll-up of the national policy, not just a supplemental policy that might require coordination between the national insurer and the private insurer.
To increase competition and motivate a drive to increase in the value delivered to the consumer, the national policy must allow for insurance policies to be allowed across State borders. This means that insurance companies that offer health insurance will have to be accredited at the national level much like financial institutions are today.
Naturally, discounts would be allowed for those who live healthier lifestyles or are otherwise lower risk (as is with every other insurance offering).
3) Tort Reform
Let’s face it, Medicine and Healthcare is an inexact science – and always will be. Therefore, no serious discussion about containing healthcare costs can be had without discussing the need for tort reform. And my personal belief is that tort reform will improve the quality of care whilst simultaneously reducing the cost of healthcare delivery.
It would increase the quality of healthcare by eliminating the fear associated with what the healthcare provider might say to whom, and under what circumstances. For instance, the doctor might be more blunt in offering an opinion. The patient won’t have to ask in a round-about manner such as, “if it were you, or your family member” – they can just ask, “What do you think I should do and why do you think that?”
Tort reform would also facilitate the learning of experiences. “If something goes wrong, why did it go wrong? What can be learned from what went wrong? How can I share the lessons learned so that others might not make the same mistake?” This open, honest and collaborative knowledge-sharing and building is non-existent under the present circumstances – so mistakes happen again and again. Best-practices are never established and replicated. What is built is a medical industry that is not transparent and one which establishes hiding and secrecy as the expected norm – it’s perverse.
Tort reform would help to eliminate the costs associated with unnecessary healthcare which is provided only to protect against litigation – but otherwise not required.
But the consumer protections offered by the opportunity to litigate cannot be eliminated otherwise all responsibility and accountability of the healthcare industry would also be eliminated. Therefore, I would propose that there be a hard definition established for what constitutes “negligence” versus “gross negligence”. Under;
- “Negligence” – any award from litigation will be limited to actual loss sustained (including that of future earnings), but would specifically exclude “punitive damages” including “pain and suffering”.
- “Gross-Negligence” – is a much higher threshold to prove. But if proven, would allow for punitive damages to be awarded, including “pain and suffering”.
Also, because the cases are often very complex and the lawyers can play on the sympathy of juries (and have), I would also require that any case of medical malpractice be tried before a Judge alone (without a jury) – with the opportunity for both sides to appeal any verdict.
4) Outcome-Based Reward System
And finally, I would re-orient the system of award in healthcare from a focus on the “inputs” (i.e. services provided) to the “outputs” (i.e. results achieved). Presently, if a healthcare provider is incorrect, or otherwise fails to have a positive effect on a situation, they get compensated anyway. There is no incentive (other than the threat of being sued) to provide the right care, in the right manner, the first time (or even the second, etc…).
If the system could be effectively re-oriented to reward outcomes – for example, no return visits for the same or related ailment within a 60-day period – then the costs of providing healthcare would be greatly reduced.
Discharge:
I believe these could all be reasonable and pragmatic “first steps” that can be enacted and deployed in fairly short order – if only the politicians can stop politicking and the lawyers can stop lawyering for just a few moments, and concentrate on the good of the nation and its people (instead of themselves) for a change.
 Paris is the Founder and Chairman of the XONITEK Group of Companies; an international management consultancy firm specializing in all disciplines related to Operational Excellence, the continuous and deliberate improvement of company performance AND the circumstances of those who work there – to pursue “Operational Excellence by Design” and not by coincidence.
Paris is the Founder and Chairman of the XONITEK Group of Companies; an international management consultancy firm specializing in all disciplines related to Operational Excellence, the continuous and deliberate improvement of company performance AND the circumstances of those who work there – to pursue “Operational Excellence by Design” and not by coincidence.
He is also the Founder of the Operational Excellence Society, with hundreds of members and several Chapters located around the world, as well as the Owner of the Operational Excellence Group on Linked-In, with over 25,000 members.
For more information on Paris, please check his Linked-In Profile at: http://de.linkedin.com/in/josephparis